Understanding Fibromyalgia: Deets On A Journey Through History, Effects, and Pain
Deets On Rights Of Disabled Americans
Understanding Fibromyalgia: Deets On A Journey Through History, Effects, and Pain
Understanding Fibromyalgia: Deets On A Journey Through History, Effects, and Pain
Fibromyalgia, a condition characterized by widespread musculoskeletal pain, fatigue, and tenderness in localized areas, has been a part of human history for centuries. Despite its long presence, the condition has often been misunderstood, misdiagnosed, and even dismissed. Today, we recognize fibromyalgia as a legitimate and debilitating condition that significantly impacts the lives of those who suffer from it. This chapter aims to shed light on the history, effects, and immense pain caused by fibromyalgia, illustrating how it can be a profoundly disabling condition.
Fibromyalgia's historical journey is one of gradual recognition and evolving understanding. For years, those suffering from the condition were often dismissed or labeled as having psychosomatic issues. The lack of visible signs and objective tests made it challenging for the medical community to validate the suffering of patients, leading to frustration and a sense of isolation for many.
However, as medical science advanced, so did our comprehension of fibromyalgia. The term itself, derived from Latin and Greek words meaning "fibrous tissues," "muscle," and "pain," hints at the complex and multifaceted nature of the condition. With a growing body of research and improved diagnostic criteria, fibromyalgia has gained legitimacy and visibility in the medical field.
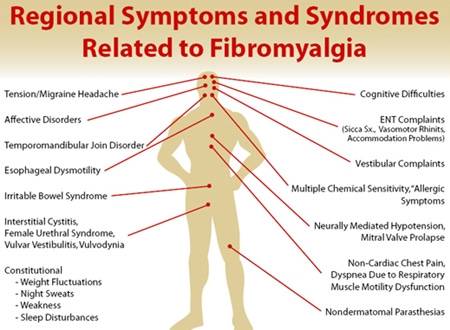
The effects of fibromyalgia extend beyond physical pain, influencing every aspect of an individual's life. The constant, pervasive pain is often accompanied by overwhelming fatigue, cognitive difficulties, and a host of other symptoms that vary from person to person. This constellation of symptoms can make everyday tasks seem insurmountable, significantly reducing the quality of life.
Understanding the nature of fibromyalgia's pain is crucial. The condition is believed to involve abnormal pain processing in the central nervous system, leading to an amplified perception of pain. This means that sufferers might experience heightened pain from stimuli that others might find only mildly uncomfortable. This pain is not just a physical experience but has deep emotional and psychological ramifications, contributing to conditions like depression and anxiety.
Recognizing fibromyalgia as a disabling condition is essential in providing appropriate support and accommodations for those affected. In many parts of the world, including the United States, fibromyalgia is becoming acknowledged as a legitimate reason for disability benefits, given its profound impact on an individual's ability to function and maintain employment. The unpredictable nature of the condition, with its flare-ups and remissions, adds to the complexity of managing daily life and work responsibilities.
In this chapter, we will explore the history of fibromyalgia, delve into the myriad effects it has on sufferers, and discuss the profound pain it causes. By increasing awareness and understanding of fibromyalgia, we can foster greater empathy and support for those living with this challenging condition. Through continued research and advocacy, there is hope for improved treatments and better quality of life for all affected by fibromyalgia.
A Brief History of Fibromyalgia
The history of fibromyalgia is a story of evolving understanding and gradual acceptance within the medical community. While the symptoms of fibromyalgia have been described for centuries, it is only in recent decades that the condition has been formally recognized and studied.
Early Descriptions and Terminology
The earliest known descriptions of a condition resembling fibromyalgia date back to the 16th century. In 1592, the French physician Guillaume de Baillou wrote about "muscular rheumatism," which exhibited symptoms similar to those of fibromyalgia. However, these early observations were often vague and lacked the specificity needed for a precise diagnosis.
In the 19th century, the Scottish surgeon Dr. William Balfour made significant strides in understanding fibromyalgia. In 1816, he described patients with tender points in their muscles and connective tissues, a hallmark of fibromyalgia. Balfour's work laid the foundation for future research, but the condition was still largely misunderstood and often attributed to psychological factors.
From "Fibrositis" to "Fibromyalgia"
In the early 20th century, the term "fibrositis" was introduced by Sir William Gowers, a British neurologist. He used this term to describe a condition characterized by pain and stiffness in the muscles and soft tissues. The suffix "-itis" implied inflammation, but as research progressed, it became clear that inflammation was not a primary feature of the condition.
The 1940s and 1950s saw further developments in the understanding of fibrositis, but the lack of objective diagnostic criteria continued to hinder progress. Patients were often misdiagnosed with conditions such as rheumatoid arthritis or labeled as having psychosomatic disorders.
It wasn't until the 1970s that the term "fibromyalgia" began to emerge. Researchers recognized that the pain and tenderness experienced by patients were not due to inflammation but rather abnormalities in pain processing. The new term, combining "fibro" (fibrous tissues), "myo" (muscle), and "algia" (pain), more accurately reflected the condition's nature.
Establishing Diagnostic Criteria
A significant milestone in the history of fibromyalgia came in 1990 when the American College of Rheumatology (ACR) established the first formal diagnostic criteria for the condition. These criteria included:
Widespread Pain: Pain that affects all four quadrants of the body and lasts for at least three months.
Tender Points: The presence of tenderness in at least 11 of 18 specific points on the body when pressure is applied.
These criteria were instrumental in validating fibromyalgia as a legitimate medical condition and provided a framework for diagnosis and research. The establishment of these criteria also helped differentiate fibromyalgia from other rheumatic and musculoskeletal disorders.
Advances in Research and Recognition
Since the 1990s, research on fibromyalgia has advanced significantly. Studies have shown that fibromyalgia is associated with abnormalities in the central nervous system's pain processing pathways. Patients with fibromyalgia have increased levels of certain neurotransmitters that amplify pain signals and decreased levels of substances that inhibit pain.
In 2007, the U.S. Food and Drug Administration (FDA) approved the first medication specifically for treating fibromyalgia. This marked a turning point in the management of the condition, providing patients with targeted treatment options.
Despite these advances, fibromyalgia remains a complex and often misunderstood condition. Many patients still face skepticism from healthcare providers and struggle to obtain accurate diagnoses and effective treatments. Advocacy and education are crucial in raising awareness and improving the lives of those affected by fibromyalgia.
The history of fibromyalgia is one of perseverance and progress. From early descriptions of "muscular rheumatism" to the establishment of formal diagnostic criteria, our understanding of fibromyalgia has come a long way. Continued research and advocacy are essential in uncovering the underlying mechanisms of the condition and developing more effective treatments. By recognizing and validating the experiences of those with fibromyalgia, we can foster a more compassionate and supportive approach to this challenging condition.
How Fibromyalgia Can Be Triggered
Fibromyalgia is a complex condition, and its exact cause remains unknown. However, researchers have identified several factors that can trigger or exacerbate the symptoms of fibromyalgia. Understanding these triggers is crucial for managing the condition and improving the quality of life for those affected. Here are some of the most common triggers associated with fibromyalgia:
Physical Trauma
Physical trauma, such as a car accident, surgery, or a significant injury, is often reported as a trigger for fibromyalgia. The stress and physical strain from these events can lead to the onset of symptoms. This connection suggests that the body's response to trauma, possibly involving changes in the nervous system, might play a role in developing fibromyalgia.
Infections
Certain infections have been linked to the development of fibromyalgia. For instance, illnesses like Epstein-Barr virus, Lyme disease, and other viral or bacterial infections can trigger the onset of fibromyalgia symptoms. The body's immune response to these infections might contribute to changes in the nervous system that lead to chronic pain and fatigue.
Emotional Stress
Emotional or psychological stress is a well-documented trigger for fibromyalgia. Stressful events such as the loss of a loved one, divorce, or other significant life changes can precipitate the onset of fibromyalgia. Chronic stress can lead to changes in the body's pain processing pathways and exacerbate symptoms in those already diagnosed with the condition.
Genetics
There is evidence to suggest that genetics play a role in fibromyalgia. The condition tends to run in families, indicating a possible genetic predisposition. While a specific gene has not been identified, researchers believe that a combination of genetic factors might make some individuals more susceptible to developing fibromyalgia after exposure to certain triggers.
Hormonal Changes
Hormonal fluctuations, particularly those related to the endocrine system, can trigger fibromyalgia symptoms. Women, who are more likely to be diagnosed with fibromyalgia, often report symptom onset or worsening during periods of hormonal change such as menopause, pregnancy, or menstrual cycles. Hormonal imbalances can affect pain sensitivity and the overall functioning of the nervous system.
Sleep Disturbances
Chronic sleep disturbances are both a symptom and a potential trigger for fibromyalgia. Poor sleep quality can lead to increased pain sensitivity and fatigue, creating a vicious cycle where lack of sleep exacerbates symptoms, and the symptoms themselves prevent restful sleep. Ensuring proper sleep hygiene and addressing sleep disorders like sleep apnea can help manage fibromyalgia symptoms.
Environmental Factors
Exposure to certain environmental factors, such as extreme weather conditions, changes in climate, and pollution, can trigger fibromyalgia symptoms. Sensitivity to temperature changes and humidity levels is common among fibromyalgia sufferers, with many reporting flare-ups during cold, damp weather or extreme heat.
Fibromyalgia is a multifaceted condition with a variety of potential triggers. While the exact cause remains elusive, understanding these triggers can help individuals manage their symptoms more effectively. By identifying and avoiding specific triggers, those with fibromyalgia can improve their quality of life and reduce the frequency and severity of flare-ups. As research continues, we hope to gain a clearer understanding of the mechanisms behind these triggers, paving the way for more targeted and effective treatments.
Can COVID-19 Trigger Fibromyalgia?
The COVID-19 pandemic has brought to light numerous long-term health consequences for those who have contracted the virus. Among the various post-viral syndromes reported, there is growing evidence that COVID-19 may act as a trigger for fibromyalgia or exacerbate existing symptoms in individuals already diagnosed with the condition.
Post-Viral Syndrome and Fibromyalgia
Post-viral syndrome, characterized by lingering symptoms following a viral infection, shares many similarities with fibromyalgia. Symptoms such as chronic fatigue, widespread pain, and cognitive difficulties (often referred to as "brain fog") are common in both conditions. COVID-19, caused by the SARS-CoV-2 virus, has been associated with a range of long-term symptoms collectively known as "Long COVID" or post-acute sequelae of SARS-CoV-2 infection (PASC).
How COVID-19 Might Trigger Fibromyalgia
Immune System Response: The body's immune response to COVID-19 can cause widespread inflammation and changes in pain perception. The cytokine storm, an excessive immune response observed in some COVID-19 patients, can lead to systemic inflammation, which might contribute to the development of fibromyalgia.
Nervous System Impact: COVID-19 can affect the central nervous system, leading to neurological symptoms and potentially altering pain processing pathways. This disruption in the nervous system could trigger the onset of fibromyalgia symptoms, such as chronic pain and fatigue.
Psychological Stress: The psychological impact of COVID-19, including anxiety, depression, and stress from illness, quarantine, and social isolation, can also act as a trigger for fibromyalgia. Emotional stress is a well-known factor in the onset and exacerbation of fibromyalgia symptoms.
Persistent Inflammation: Chronic inflammation resulting from a COVID-19 infection might also play a role. Ongoing inflammation can lead to prolonged pain and fatigue, which are characteristic of fibromyalgia. The prolonged recovery period and continued immune activation in some COVID-19 survivors may set the stage for developing fibromyalgia.
Case Reports and Emerging Evidence
There are increasing reports and studies indicating a link between COVID-19 and the development of fibromyalgia-like symptoms. Some COVID-19 survivors have reported new-onset widespread pain, fatigue, and other symptoms consistent with fibromyalgia months after their initial infection. While these observations are still under investigation, they suggest that COVID-19 could potentially act as a catalyst for fibromyalgia in susceptible individuals.
Managing Fibromyalgia Post-COVID-19
For individuals experiencing fibromyalgia-like symptoms following a COVID-19 infection, management strategies should include:
Medical Evaluation: Consult a healthcare provider to rule out other potential causes and confirm a diagnosis of fibromyalgia.
Pain Management: Use medications, physical therapy, and other pain management strategies to alleviate symptoms.
Mental Health Support: Address the psychological impact of both COVID-19 and fibromyalgia through counseling, support groups, and stress management techniques.
Lifestyle Modifications: Implement changes such as regular, gentle exercise, a balanced diet, and good sleep hygiene to manage symptoms effectively.
While more research is needed to fully understand the relationship between COVID-19 and fibromyalgia, current evidence suggests that the virus may trigger or worsen fibromyalgia symptoms in some individuals. Recognizing this potential link is crucial for providing appropriate care and support to those affected. As the medical community continues to study the long-term effects of COVID-19, greater insight into its role in triggering fibromyalgia will likely emerge, paving the way for better management and treatment strategies.
The Effects of Fibromyalgia
Fibromyalgia is a complex and multifaceted condition that affects various aspects of a person's life. The symptoms of fibromyalgia can be pervasive and debilitating, impacting physical, mental, and emotional well-being. Understanding these effects is crucial for providing comprehensive care and support to those living with this condition. Here, we delve into the diverse and profound effects of fibromyalgia.
Physical Effects
Widespread Pain: The hallmark symptom of fibromyalgia is widespread musculoskeletal pain. This pain is often described as a constant, dull ache that affects multiple regions of the body. It typically occurs on both sides of the body, above and below the waist. The intensity of the pain can vary from mild to severe and may fluctuate throughout the day or from day to day.
Tender Points: Individuals with fibromyalgia often experience tenderness in specific areas known as tender points. These are localized spots on the body that are painful when pressure is applied. Common tender points include the back of the head, tops of the shoulders, upper chest, hips, and knees.
Fatigue: Chronic fatigue is another common symptom of fibromyalgia. This fatigue is not simply a feeling of being tired but is often described as an overwhelming exhaustion that does not improve with rest. It can significantly impair daily functioning and reduce the ability to engage in normal activities.
Sleep Disturbances: Many people with fibromyalgia experience sleep disturbances, including difficulty falling asleep, staying asleep, and non-restorative sleep. Conditions like restless legs syndrome and sleep apnea are also more prevalent among fibromyalgia patients. Poor sleep quality exacerbates other symptoms, such as pain and fatigue, creating a vicious cycle.
Stiffness: Morning stiffness is a common complaint among fibromyalgia sufferers. This stiffness can last for several hours and may occur after periods of inactivity. It can make it difficult to move and perform everyday tasks.
Other Physical Symptoms: Fibromyalgia can also cause headaches, migraines, irritable bowel syndrome (IBS), and temporomandibular joint disorder (TMJ). Sensitivity to temperature changes, light, noise, and certain foods is also frequently reported.
Cognitive Effects
Cognitive Dysfunction: Often referred to as "fibro fog," cognitive dysfunction in fibromyalgia can include problems with memory, attention, and concentration. Patients may struggle with tasks that require mental clarity, such as following conversations, remembering details, and organizing thoughts.
Slowed Thinking: Some individuals experience slowed thinking and difficulty processing information quickly. This can impact decision-making and the ability to perform tasks efficiently, leading to frustration and reduced productivity.
Emotional and Psychological Effects
Depression: Depression is common among those with fibromyalgia. The chronic pain and fatigue associated with the condition can lead to feelings of hopelessness, sadness, and a loss of interest in activities once enjoyed. The stigma and misunderstanding surrounding fibromyalgia can also contribute to feelings of isolation and depression.
Anxiety: Anxiety is another frequent companion of fibromyalgia. The unpredictable nature of the condition, with its flare-ups and remissions, can create a constant state of worry and fear about when the next episode of severe pain or fatigue will occur.
Stress: The daily challenges of living with fibromyalgia, including managing symptoms, attending medical appointments, and dealing with the impact on work and personal life, can lead to significant stress. Chronic stress, in turn, can exacerbate fibromyalgia symptoms, creating a harmful cycle.
Social and Occupational Effects
Impact on Work: Fibromyalgia can significantly affect an individual's ability to maintain employment. Chronic pain, fatigue, and cognitive dysfunction can make it difficult to meet job demands, leading to reduced work hours, frequent absences, or even job loss. Many individuals with fibromyalgia may need to seek accommodations or change their career paths to manage their symptoms effectively.
Social Isolation: The symptoms of fibromyalgia can limit social interactions and participation in activities. Pain and fatigue may prevent individuals from attending social gatherings, participating in hobbies, or engaging in physical activities, leading to a sense of isolation and loneliness.
Strain on Relationships: Fibromyalgia can place a strain on relationships with family, friends, and partners. Loved ones may have difficulty understanding the condition and the limitations it imposes. The need for support and understanding from those close to the individual with fibromyalgia is crucial for their emotional well-being.
The effects of fibromyalgia are far-reaching and multifaceted, impacting physical health, cognitive function, emotional well-being, and social and occupational life. Understanding these effects is essential for providing comprehensive care and support to individuals with fibromyalgia. By recognizing the diverse ways in which fibromyalgia can affect a person's life, we can foster greater empathy and develop more effective strategies for managing this challenging condition. Through continued research, advocacy, and education, we can improve the quality of life for those living with fibromyalgia and work towards better treatments and support systems.
The Pain of Fibromyalgia
Fibromyalgia is primarily characterized by chronic, widespread pain that significantly impacts the lives of those who suffer from it. This pain is not merely a symptom; it is a multifaceted experience that encompasses physical, emotional, and psychological dimensions. Understanding the nature and impact of this pain is crucial for both patients and healthcare providers in managing the condition effectively.
Nature of Fibromyalgia Pain
Widespread Musculoskeletal Pain: The most prominent feature of fibromyalgia is widespread musculoskeletal pain. This pain is often described as a persistent, dull ache that affects multiple areas of the body, typically occurring on both sides of the body and above and below the waist. The pain can vary in intensity from mild to severe and may be constant or fluctuate over time.
Tender Points: Individuals with fibromyalgia often experience tenderness in specific areas of the body, known as tender points. These are localized spots that are painful when pressure is applied. Common tender points include the back of the head, the tops of the shoulders, the upper chest, the outer elbows, the hips, and the inner knees. The presence of tender points is a key diagnostic criterion for fibromyalgia.
Deep, Aching Pain: The pain associated with fibromyalgia is often described as deep and aching. It can feel like a muscle strain or soreness that does not go away. This type of pain can make it difficult to perform everyday activities and can significantly reduce the quality of life.
Neuropathic Pain: Some individuals with fibromyalgia experience neuropathic pain, which is pain that arises from nerve damage or dysfunction. This can include sensations such as burning, tingling, numbness, and shooting pain. Neuropathic pain can be particularly challenging to manage and can add to the overall burden of fibromyalgia.
Factors Influencing Pain Perception
Central Sensitization: Central sensitization is believed to be a key mechanism underlying fibromyalgia pain. This phenomenon happens when the central nervous system becomes overly sensitive to pain signals. As a result, individuals with fibromyalgia may experience pain from stimuli that would not normally be painful, a condition known as allodynia. Additionally, they may have an exaggerated response to painful stimuli, known as hyperalgesia.
Neurotransmitter Imbalances: Research has shown that individuals with fibromyalgia often have imbalances in certain neurotransmitters involved in pain processing. For example, they may have elevated levels of substance P, which enhances pain perception, and reduced levels of serotonin and norepinephrine, which inhibit pain. These imbalances contribute to the heightened pain sensitivity seen in fibromyalgia.
Sleep Disturbances: Poor sleep quality is common in fibromyalgia and can exacerbate pain. Non-restorative sleep and sleep disorders such as restless legs syndrome and sleep apnea are frequently reported. Lack of restorative sleep impairs the body's ability to repair and regenerate, leading to increased pain and fatigue.
Emotional and Psychological Stress: Emotional and psychological stress can significantly influence the perception of pain in fibromyalgia. Anxiety, depression, and chronic stress can amplify pain signals and reduce pain tolerance. The bidirectional relationship between pain and emotional distress creates a vicious cycle, where pain leads to stress and stress, in turn, exacerbates pain.
Impact of Fibromyalgia Pain
Physical Functioning: Chronic pain can severely impact physical functioning, making it difficult to perform daily activities such as walking, climbing stairs, lifting objects, and even simple tasks like dressing or bathing. The constant pain and stiffness can lead to a sedentary lifestyle, which further contributes to muscle weakness and reduced physical capacity.
Mental Health: The relentless nature of fibromyalgia pain can take a toll on mental health. Many individuals with fibromyalgia experience depression and anxiety, which can worsen their pain perception and overall quality of life. The sense of hopelessness and frustration that often accompanies chronic pain can lead to feelings of isolation and helplessness.
Social and Occupational Life: The pain and fatigue associated with fibromyalgia can interfere with social interactions and relationships. Individuals may withdraw from social activities and hobbies they once enjoyed due to the debilitating pain. Additionally, maintaining employment can be challenging, leading to financial strain and further stress.
Quality of Life: Overall, the chronic pain of fibromyalgia significantly reduces the quality of life. The constant battle with pain can overshadow all aspects of life, from physical health to emotional well-being and social functioning. Effective pain management is crucial in improving the quality of life for those with fibromyalgia.
Medications for Managing Fibromyalgia Pain
Managing fibromyalgia pain often requires a multifaceted approach, and medications can play a crucial role in alleviating symptoms. There is no single medication that works for everyone, and treatment often involves a combination of different drugs tailored to the individual's specific symptoms and needs. Here, we explore the various types of medications commonly used to manage fibromyalgia pain.
Pain Relievers
Over-the-Counter Pain Relievers:
Acetaminophen (Tylenol): This medication can help relieve mild to moderate pain but does not address inflammation.
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): Drugs like ibuprofen (Advil, Motrin) and naproxen (Aleve) can help reduce pain and inflammation. However, their effectiveness in fibromyalgia is limited, and long-term use can lead to gastrointestinal issues and other side effects.
Prescription Pain Relievers:
Tramadol (Ultram): This prescription pain reliever is sometimes used for managing fibromyalgia pain. It works on the central nervous system to relieve moderate to severe pain. However, it can be habit-forming and should be used with caution.
Antidepressants
Tricyclic Antidepressants:
Amitriptyline (Elavil): This medication helps reduce pain, improve sleep, and alleviate depression. It works by increasing the levels of certain neurotransmitters that help regulate pain in the brain.
Nortriptyline (Pamelor): Similar to amitriptyline, nortriptyline is another tricyclic antidepressant used to manage pain and improve sleep quality in fibromyalgia patients.
Serotonin and Norepinephrine Reuptake Inhibitors (SNRIs):
Duloxetine (Cymbalta): Approved by the FDA for the treatment of fibromyalgia, duloxetine helps reduce pain and improve function by increasing the levels of serotonin and norepinephrine in the brain.
Milnacipran (Savella): Another SNRI specifically approved for fibromyalgia, milnacipran helps manage pain and fatigue by enhancing neurotransmitter levels.
Selective Serotonin Reuptake Inhibitors (SSRIs):
Fluoxetine (Prozac): Although not specifically approved for fibromyalgia, fluoxetine can help manage depression and anxiety, which can indirectly alleviate fibromyalgia symptoms.
Sertraline (Zoloft): Another SSRI that can help improve mood and manage depression associated with fibromyalgia.
Anti-Seizure Medications
Gabapentin (Neurontin): Gabapentin is used to reduce nerve pain in fibromyalgia by altering the way the brain and nerves process pain signals. It can help alleviate pain and improve sleep.
Pregabalin (Lyrica): Approved by the FDA specifically for fibromyalgia, pregabalin works similarly to gabapentin. It reduces pain, improves sleep, and decreases the sensitivity of nerves involved in pain transmission.
Muscle Relaxants
Cyclobenzaprine (Flexeril): This muscle relaxant is often used to treat muscle spasms associated with fibromyalgia. It can help reduce pain and improve sleep quality by relaxing muscles and alleviating tension.
Sleep Aids
Trazodone: Although primarily used as an antidepressant, trazodone is often prescribed in low doses to help improve sleep in fibromyalgia patients. It can help manage insomnia and enhance sleep quality without being as habit-forming as other sleep medications.
Zolpidem (Ambien): A short-term sleep aid that can help with severe sleep disturbances. It should be used with caution due to the potential for dependence and side effects such as dizziness and daytime drowsiness.
Medications for Associated Symptoms
Irritable Bowel Syndrome (IBS) Medications:
Loperamide (Imodium): For diarrhea.
Polyethylene glycol (MiraLAX): For constipation.
Headache Medications:
Triptans: For migraine headaches.
Beta-blockers and calcium channel blockers: For preventing chronic headaches and migraines.
Combination Therapy
Many individuals with fibromyalgia benefit from a combination of medications tailored to their specific symptoms. For example, a patient might use an antidepressant to manage mood and pain, an anti-seizure medication to reduce nerve pain, and a muscle relaxant to ease muscle tension. This multifaceted approach can address the different aspects of fibromyalgia and provide more comprehensive relief.
Monitoring and Adjustments
Finding the right combination and dosage of medications often requires careful monitoring and adjustments by a healthcare provider. It's important to start with lower doses and gradually increase as needed while monitoring for side effects. Regular follow-up appointments are essential to ensure that the medications are effective and to make any necessary changes.
Non-Pharmacological Interventions
Medications are just one part of the comprehensive management of fibromyalgia. Non-pharmacological interventions such as physical therapy, cognitive-behavioral therapy, exercise, and lifestyle modifications play a crucial role in managing symptoms and improving quality of life. Combining these approaches with appropriate medications can provide the best outcomes for individuals with fibromyalgia.
Medications are a key component in managing the complex symptoms of fibromyalgia. From pain relievers and antidepressants to anti-seizure drugs and muscle relaxants, various medications can help alleviate pain, improve sleep, and enhance overall well-being. A personalized approach, often involving a combination of different medications and non-pharmacological treatments, is essential for effectively managing this challenging condition. With ongoing research and a better understanding of fibromyalgia, more targeted and effective treatments will continue to emerge, offering hope and relief to those affected by this debilitating condition.
Exploring the Potential of THC for Fibromyalgia Relief

Tetrahydrocannabinol (THC), the psychoactive component of cannabis, has garnered attention as a potential treatment for fibromyalgia symptoms. As traditional treatments often provide limited relief for many patients, alternative therapies like THC are being explored for their efficacy in managing the chronic pain, fatigue, and other symptoms associated with fibromyalgia. This section examines the potential benefits and drawbacks of THC for fibromyalgia patients based on current research and anecdotal evidence.
Potential Benefits of THC for Fibromyalgia
Pain Relief: THC is known for its analgesic properties, making it a potential option for managing the chronic pain associated with fibromyalgia. Some studies and patient reports suggest that THC can help reduce pain intensity and improve overall comfort.
Improved Sleep: Many fibromyalgia patients struggle with sleep disturbances, including difficulty falling asleep, staying asleep, and non-restorative sleep. THC may help improve sleep quality and duration by promoting relaxation and reducing pain, which can contribute to better rest.
Reduction in Muscle Spasms: Muscle spasms and stiffness are common symptoms of fibromyalgia. THC may help alleviate these symptoms by relaxing muscles and reducing spasms, thereby improving mobility and comfort.
Enhanced Mood: Chronic pain and fatigue can lead to depression, anxiety, and overall poor mental health. THC has been reported to have mood-enhancing effects, which can help improve the emotional well-being of fibromyalgia patients.
Anti-Inflammatory Effects: While inflammation is not a primary feature of fibromyalgia, it can contribute to pain and discomfort. THC has anti-inflammatory properties that may help reduce inflammation and associated pain in some patients.
Potential Drawbacks of THC for Fibromyalgia
Psychoactive Effects: The psychoactive nature of THC can lead to side effects such as dizziness, euphoria, paranoia, and impaired cognitive function. These effects can be particularly challenging for individuals already experiencing "fibro fog" and cognitive difficulties.
Legal and Accessibility Issues: The legal status of THC varies widely by location, which can affect its availability and accessibility for fibromyalgia patients. In some regions, obtaining THC legally can be difficult, and its use may be restricted.
Tolerance and Dependence: Regular use of THC can lead to tolerance, requiring higher doses to achieve the same effects. There is also a risk of developing dependence, which can complicate treatment and management of fibromyalgia symptoms.
Variable Efficacy: The effectiveness of THC in managing fibromyalgia symptoms can vary significantly from person to person. Some patients may experience substantial relief, while others may find little to no benefit. This variability makes it important for patients to work closely with healthcare providers to determine the best approach.
Side Effects: Common side effects of THC include dry mouth, increased heart rate, and impaired short-term memory. These side effects can be particularly troublesome for fibromyalgia patients, who may already be dealing with similar symptoms.
Research and Evidence
Research on the effects of THC on fibromyalgia is still in its early stages, and more studies are needed to establish its efficacy and safety. Some clinical trials and observational studies have shown promising results, indicating that THC may help reduce pain and improve sleep quality in fibromyalgia patients. However, the long-term effects and potential risks are not yet fully understood.
A notable study published in the Journal of Clinical Rheumatology found that a combination of THC and cannabidiol (CBD) reduced pain and improved quality of life in fibromyalgia patients. Another study published in Pain Medicine reported that fibromyalgia patients who used medical cannabis experienced significant reductions in pain and stiffness.
THC shows promise as a potential treatment for managing fibromyalgia symptoms, particularly pain and sleep disturbances. However, its psychoactive effects, legal status, and variable efficacy make it essential for patients to approach its use cautiously. Collaborating with healthcare providers to tailor a treatment plan that considers individual responses and potential risks is crucial.
As research continues to explore the benefits and drawbacks of THC for fibromyalgia, patients and healthcare providers alike should stay informed about new findings and developments. With a comprehensive and personalized approach, THC may offer relief for some fibromyalgia patients, improving their overall quality of life.
The Role of Ketamine in Managing Fibromyalgia Symptoms
Ketamine, primarily known as an anesthetic and dissociative drug, has garnered attention for its potential therapeutic effects in treating chronic pain conditions, including fibromyalgia. Research and clinical reports suggest that ketamine can help alleviate some of the debilitating symptoms of fibromyalgia, particularly chronic pain. This section explores the evidence supporting the use of ketamine for fibromyalgia, its mechanisms of action, and the potential benefits and drawbacks.
Research and Clinical Findings
Pain Relief:
Clinical Studies: Multiple studies have highlighted ketamine’s potential in reducing pain among fibromyalgia patients. A notable small-scale study from 2007 reported that approximately two-thirds of fibromyalgia patients responded positively to ketamine, experiencing significant pain reduction. This study suggested that ketamine might enhance cerebral blood flow, thereby contributing to its analgesic effects.
Long-term Effects: While some patients experience substantial short-term pain relief, the duration of ketamine's effects can vary. Some individuals report weeks of reduced pain following treatment, whereas others require repeated infusions to maintain benefits. A 2011 study using S(+)-ketamine found that about one-third of patients experienced a 50% reduction in pain, although the effects were not long-lasting.
Mechanism of Action: Ketamine functions as an NMDA (N-methyl-D-aspartate) receptor antagonist. NMDA receptors play a crucial role in pain transmission and central sensitization, which is a significant factor in fibromyalgia. By blocking these receptors, ketamine helps to modulate pain pathways, reducing the heightened pain sensitivity associated with fibromyalgia. Additionally, ketamine’s impact on neurotransmitter systems, including increasing glutamate levels, may contribute to its pain-relieving and antidepressant effects.
Cognitive and Emotional Benefits: Beyond its analgesic properties, ketamine is noted for its rapid antidepressant effects. Given the high prevalence of depression and anxiety among fibromyalgia patients, ketamine’s ability to improve mood and cognitive function can significantly enhance overall quality of life. Improved mental health can indirectly reduce the perception of pain and help patients manage their symptoms more effectively.
Potential Drawbacks and Considerations
Side Effects: Ketamine can cause several side effects, including dissociation, dizziness, nausea, and increased blood pressure. These effects can be particularly challenging for fibromyalgia patients, who may already be dealing with significant discomfort and cognitive issues. The psychoactive properties of ketamine necessitate careful monitoring during treatment to manage these side effects effectively.
Variable Efficacy: The response to ketamine treatment can vary significantly among patients. While some experience substantial relief, others may find limited benefits. The variability in response also extends to the duration of pain relief, with some patients requiring ongoing treatment to maintain the effects. This inconsistency underscores the importance of personalized treatment plans and close monitoring by healthcare providers.
Cost and Accessibility: Ketamine infusions can be expensive, and their cost is not always covered by insurance. Additionally, access to treatment may be limited by geographical location and the availability of clinics offering ketamine therapy. The logistical challenges associated with receiving ketamine treatment can pose significant barriers for some patients.
Ketamine shows promise as a potential treatment for managing fibromyalgia symptoms, particularly chronic pain and associated mood disorders. Its ability to modulate pain pathways and provide rapid relief makes it a valuable option, especially for those who have not responded well to traditional treatments. However, due to its side effects, variable efficacy, and cost, it is essential for patients to consult with healthcare providers to determine if ketamine therapy is appropriate for their specific situation. More extensive and rigorous studies are needed to fully understand the long-term effects and optimal use of ketamine for fibromyalgia.
The Role of Psychedelics in Managing Fibromyalgia Symptoms
The use of psychedelics such as psilocybin, MDMA, and LSD for therapeutic purposes has gained increasing interest in recent years. While traditionally associated with recreational use, these substances are being studied for their potential to alleviate various chronic conditions, including fibromyalgia. This section explores the potential benefits and challenges of using psychedelics to manage fibromyalgia symptoms based on emerging research and anecdotal evidence.
Psilocybin
Potential Benefits:
Pain Reduction: Psilocybin, the active compound in magic mushrooms, has been shown to modulate pain perception. Some studies suggest it may help reduce chronic pain by altering the brain's pain processing pathways.
Mood Enhancement: Psilocybin has significant effects on mood and emotional well-being. It may help alleviate depression and anxiety, common comorbidities in fibromyalgia patients, thereby improving overall quality of life.
Neuroplasticity: Psilocybin may promote neuroplasticity, the brain's ability to reorganize itself by forming new neural connections. This could potentially help in resetting dysfunctional pain pathways.
Challenges:
Psychoactive Effects: The hallucinogenic effects of psilocybin can be intense and may cause distress or confusion in some users, particularly those with a history of mental health issues.
Legal Status: Psilocybin is classified as a Schedule I controlled substance in many countries, making it illegal and difficult to access for therapeutic purposes.
Research Limitations: While promising, research on psilocybin for fibromyalgia is still in early stages, and more extensive clinical trials are needed to establish safety and efficacy.
MDMA
Potential Benefits:
Pain Relief: MDMA, commonly known as ecstasy, has been reported to provide pain relief by increasing levels of serotonin, dopamine, and norepinephrine, neurotransmitters involved in pain modulation.
Emotional Healing: MDMA is known for its ability to enhance emotional connection and reduce fear and anxiety. For fibromyalgia patients, this could mean better coping mechanisms and reduced emotional distress associated with chronic pain.
Improved PTSD Symptoms: Some fibromyalgia patients also suffer from PTSD. MDMA-assisted therapy has shown promise in treating PTSD, which could indirectly benefit fibromyalgia patients by alleviating overlapping symptoms.
Challenges:
Neurotoxicity Concerns: There are concerns about the potential neurotoxic effects of MDMA, particularly with repeated use, which could limit its long-term applicability for fibromyalgia management.
Side Effects: MDMA can cause side effects such as increased heart rate, anxiety, dehydration, and potential for misuse.
Legal and Research Barriers: As with other psychedelics, MDMA is a Schedule I controlled substance, complicating access and research efforts.
LSD
Potential Benefits:
Pain Perception Modulation: LSD (lysergic acid diethylamide) may alter the perception of pain, potentially providing relief for fibromyalgia patients. It can induce a state of altered consciousness that might help in dissociating from chronic pain.
Mental Health Improvement: LSD has been studied for its potential to improve mood and reduce symptoms of anxiety and depression, which are often associated with fibromyalgia.
Enhanced Neuroplasticity: Like psilocybin, LSD may promote neuroplasticity, potentially aiding in the reorganization of dysfunctional pain pathways in the brain.
Challenges:
Psychoactive Effects: The strong hallucinogenic effects of LSD can be overwhelming and unpredictable, posing a risk for those with mental health vulnerabilities.
Legal Status and Accessibility: LSD is also classified as a Schedule I substance, making it illegal and difficult to obtain for therapeutic use.
Limited Research: Research on LSD for chronic pain, including fibromyalgia, is limited. More rigorous clinical trials are necessary to validate its safety and efficacy.
Psychedelics such as psilocybin, MDMA, and LSD offer intriguing potential for managing fibromyalgia symptoms, particularly in terms of pain relief, mood enhancement, and neuroplasticity. However, significant challenges remain, including legal restrictions, potential side effects, and the need for more extensive research to establish clear therapeutic protocols.
As interest in psychedelic therapy grows, it is crucial for both patients and healthcare providers to stay informed about the latest developments and research findings. With careful consideration and a focus on safety, psychedelics could emerge as a valuable addition to the array of treatment options available for fibromyalgia, offering hope for improved quality of life for those affected by this debilitating condition.
Fibromyalgia as a Disabling Condition
Fibromyalgia is recognized as a debilitating and chronic condition that can significantly impair an individual's ability to function in daily life. The widespread pain, fatigue, cognitive difficulties, and emotional distress associated with fibromyalgia can make it difficult for individuals to perform routine activities, maintain employment, and engage in social interactions. Here, we explore how fibromyalgia can be a disabling condition and the various aspects that contribute to its profound impact on individuals' lives.
Impact on Daily Functioning
Physical Limitations: The chronic pain and stiffness associated with fibromyalgia can severely limit physical activities. Simple tasks such as walking, climbing stairs, lifting objects, and even personal hygiene can become challenging. The constant pain can lead to a sedentary lifestyle, further exacerbating muscle weakness and physical deconditioning.
Fatigue: Persistent fatigue is a hallmark symptom of fibromyalgia, often described as an overwhelming exhaustion that does not improve with rest. This fatigue can be so debilitating that it impairs the ability to perform everyday activities, including household chores, personal care, and social engagements. The unpredictable nature of fatigue can make planning and participating in activities difficult.
Cognitive Dysfunction: Cognitive difficulties, commonly referred to as "fibro fog," are a significant aspect of fibromyalgia. Problems with memory, attention, concentration, and mental clarity can interfere with daily tasks and responsibilities. This cognitive dysfunction can make it hard to follow conversations, remember appointments, and manage day-to-day tasks, leading to frustration and a reduced ability to function independently.
Impact on Employment
Reduced Work Capacity: The physical and cognitive symptoms of fibromyalgia can make it challenging to maintain consistent work performance. Many individuals with fibromyalgia report difficulties in fulfilling job responsibilities, meeting deadlines, and maintaining productivity. This can lead to reduced work hours, frequent absences, or the need for modified duties.
Job Loss and Financial Strain: In severe cases, individuals with fibromyalgia may be unable to continue working, leading to job loss and financial strain. The loss of income, combined with medical expenses, can create significant financial burdens. Applying for disability benefits can be a complex and lengthy process, adding to the stress and anxiety faced by individuals with fibromyalgia.
Workplace Accommodations: To remain employed, individuals with fibromyalgia may require workplace accommodations such as flexible work hours, the ability to work from home, ergonomic workstations, and additional breaks. Employers' understanding and support in providing these accommodations can significantly impact the ability of individuals with fibromyalgia to maintain employment.
Social and Emotional Impact
Social Isolation: The chronic pain and fatigue associated with fibromyalgia can limit social interactions and participation in activities. Individuals may withdraw from social gatherings, hobbies, and recreational activities due to pain and exhaustion. This social isolation can lead to feelings of loneliness and depression.
Strain on Relationships: Fibromyalgia can place a strain on relationships with family, friends, and partners. Loved ones may have difficulty understanding the condition and the limitations it imposes. The need for support and understanding from those close to the individual with fibromyalgia is crucial for their emotional well-being.
Mental Health: The emotional toll of living with fibromyalgia can be significant. Many individuals experience depression, anxiety, and stress due to the chronic nature of the condition and its impact on their lives. The sense of helplessness and frustration that often accompanies chronic pain can exacerbate mental health issues, creating a cycle of pain and emotional distress.
Recognizing Fibromyalgia as a Disability
Medical and Legal Recognition: Many medical and governmental organizations worldwide recognize fibromyalgia as a disabling condition. In the United States, the Social Security Administration (SSA) acknowledges fibromyalgia as a legitimate reason for disability benefits, provided that the condition meets specific criteria. These criteria include documented medical evidence of fibromyalgia, a history of chronic pain and fatigue, and the inability to perform substantial gainful activity.
Disability Benefits: Applying for disability benefits can provide financial support and access to healthcare services for individuals with fibromyalgia. The process typically involves providing comprehensive medical documentation, including diagnostic tests, treatment history, and assessments from healthcare providers. Obtaining disability benefits can be challenging and may require legal assistance to navigate the application and appeals process.
Advocacy and Education: Advocacy and education are crucial in raising awareness and understanding of fibromyalgia as a disabling condition. Increased public awareness can help reduce stigma, promote empathy, and encourage support for individuals with fibromyalgia. Healthcare providers, employers, and policymakers play essential roles in recognizing the impact of fibromyalgia and providing appropriate resources and accommodations.
Fibromyalgia is a chronic and debilitating condition that can significantly impair an individual's ability to function in daily life, maintain employment, and engage in social interactions. The widespread pain, fatigue, cognitive difficulties, and emotional distress associated with fibromyalgia contribute to its recognition as a disabling condition. Understanding the profound impact of fibromyalgia and providing appropriate support and accommodations are essential in improving the quality of life for those affected by this challenging condition. Through continued advocacy, education, and research, we can foster greater awareness and develop more effective strategies for managing fibromyalgia and supporting those who live with it.
Deets On Having Fibromyalgia
In 2023, after years of dead-end doctors appointments, I was finally referred to a rheumatologist. Ironically, I was sent there to be assessed for Sjögren's Syndrome. All of the biomarkers came back negative for that (even though I would later be officially diagnosed with sicca), but I was officially diagnosed with Fibromyalgia, meeting 14 out of the 18 trigger points.
I believe my first fibro flare up was after I got really, really sick in February 2020. I honestly think it was OG COVID, but tests weren’t available yet so I can’t say that for sure. I just know that for the first time in my life, I was sick for months on end having to take breathing treatments to clear my lungs. I am not and have not been asthmatic, and haven’t needed a treatment since the sickness finally lifted.
Point is, I think COVID, due to the duration and severity of my symptoms, triggered my initial fibro symptoms. And the damage COVID caused created an environment for those symptoms to take chronic hold.
While I did not expect the assessement to result in a Fibromyalgia diagnosis, a part of me was relieved to actually have a word to define my various symptoms, namely brain fog and constant, generalized pain. Further, now we could focus on treatment options.
For the first six months, the rheumatologist focused on trying to treat my dry mouth. I started with Pilocarpine until I maxed out that dosage with no improvement, at which point I was switched over to cevilimine, until I maxed out that dosage. With no real improvement for dry mouth, my rheumatologist then shifted their attention to address the pain.
The pain is constant. While it can be mild, I have no days in which my pain level is less than a 3/10, and most days easily pass 5-6/10. After months of trial and error, I currently sit at 1800 mg of gabapentin a day along with 3 mg of low dose naltrexone (batched compound). While I’m tolerating these medications, I still have had no real improvement and pain and expect for those dosages to increase at my next appointment.
I’m also on nortriptyline oral solution, but that was prescribed for depression and GI issues, so I can’t really comment on it’s usage for Fibromyalgia.
The brain fog and cognitive decline are just as debilitating as the pain. My short-term memory is shot, I can’t even decide on what to eat on most days, and I can’t remember anything for more than five minutes most of the time. And my brain just doesn’t process information at times. I can be looking at an image, and my brain is just unable to turn that image into a mental concept.
I can’t think. I can’t sleep. I have trouble eating.
I’m barely alive, and I can feel the pain and brain fog increase month over month over month.
My hope is in psychedelics, but, with them being Schedule 1, I feel like I hit a wall with my weekly Spravato (esketamine/”nasal ketamine”) sessions and am in a holding pattern until Psilocybin and/or MDMA get reclassified. The physical and mental pain causes passive suicidal ideation multiple days a week. I fear active suicidal ideation will overtake me once again if I lose my Spravato treatment. So I continue my cycle. Prescriptions. Appointments. Spravato. Prescriptions. Appointments. Spravato. Prescriptions. Appointments. Spravato…
I keep my eye out for clinical trials, but those are hard to come by for someone with my comorbidities, medical history, medications, and location. Which is another reason why I’ll be voting for Biden and Harris in November 2024. They have a plan for reclassificiation. Meanwhile, the twice indicted, twice impeached and, hopefully by the end of 2024, twice convicted, orange buffoon doesn’t give a shit about our collective mental health.
Conclusion
Fibromyalgia is a chronic and debilitating condition that affects millions of people worldwide. Despite its prevalence, fibromyalgia remains a misunderstood and often misdiagnosed illness. The widespread pain, fatigue, cognitive difficulties, and emotional distress it causes can have profound and far-reaching impacts on an individual's life. Understanding these effects is essential for providing comprehensive care and support to those living with this challenging condition.
Recognizing the Pervasive Impact of Fibromyalgia
The effects of fibromyalgia are multifaceted, influencing physical health, mental well-being, and social interactions. The persistent and widespread pain characteristic of fibromyalgia can make even the simplest daily activities seem insurmountable. This pain is not merely a symptom but a complex experience influenced by central sensitization, neurotransmitter imbalances, and other factors. Additionally, the chronic fatigue associated with fibromyalgia can lead to a significant reduction in physical activity, further exacerbating symptoms and impacting overall health.
Cognitive dysfunction, often referred to as "fibro fog," adds another layer of complexity to living with fibromyalgia. Memory issues, difficulty concentrating, and slowed thinking can interfere with daily tasks, work responsibilities, and social interactions, leading to frustration and decreased quality of life.
The Emotional and Psychological Toll
The emotional and psychological impact of fibromyalgia cannot be understated. Chronic pain and fatigue often lead to depression, anxiety, and increased stress levels. These mental health challenges can create a vicious cycle, where pain leads to emotional distress, which in turn exacerbates the perception of pain. Social isolation and strained relationships further contribute to the emotional burden, highlighting the need for comprehensive mental health support as part of fibromyalgia management.
The Need for Recognition and Support
Fibromyalgia is recognized as a disabling condition by many medical and governmental organizations worldwide. However, obtaining a diagnosis and accessing appropriate support can be a complex and lengthy process. Advocacy and education are crucial in raising awareness and understanding of fibromyalgia. Increased public awareness can help reduce stigma, promote empathy, and encourage support from healthcare providers, employers, and policymakers.
Effective Management Strategies
Managing fibromyalgia requires a multifaceted approach that includes medications, physical therapy, cognitive-behavioral therapy, and lifestyle modifications. Medications can help alleviate pain, improve sleep, and address associated symptoms such as depression and anxiety. Physical therapy and gentle exercise can improve strength, flexibility, and overall physical function. Cognitive-behavioral therapy can provide strategies for coping with pain and reducing stress, while lifestyle modifications such as maintaining a healthy diet, practicing good sleep hygiene, and engaging in mindfulness activities can help manage symptoms.
Looking Forward: Research and Advocacy
Ongoing research is essential in uncovering the underlying mechanisms of fibromyalgia and developing more effective treatments. Advances in understanding central sensitization, neurotransmitter imbalances, and genetic predispositions can pave the way for new therapeutic approaches. Advocacy efforts play a vital role in promoting research, increasing public awareness, and securing support for individuals with fibromyalgia.
A Call to Action
The journey of living with fibromyalgia is fraught with challenges, but with increased awareness, empathy, and comprehensive care, individuals with fibromyalgia can lead fulfilling lives. It is crucial for healthcare providers, policymakers, employers, and the general public to recognize the profound impact of fibromyalgia and work together to provide the necessary support and accommodations. By fostering a compassionate and informed approach, we can improve the quality of life for those affected by this condition and pave the way for a brighter future.
Final Thoughts
Fibromyalgia is more than just a medical condition; it is a lived experience that affects every aspect of an individual's life. Understanding its history, triggers, effects, and the pain it causes is essential for providing appropriate care and support. By recognizing fibromyalgia as a disabling condition and advocating for comprehensive management strategies, we can help those living with fibromyalgia navigate their daily challenges and achieve a better quality of life. Through continued research, advocacy, and education, we can foster a more supportive and empathetic environment for individuals with fibromyalgia, ultimately leading to improved outcomes and a greater sense of hope for the future.
Legal Disclaimer
The information provided in this blog post is for informational purposes only and is not intended as medical, legal, or professional advice. It is not a substitute for consultation with a qualified healthcare provider, medical professional, or legal advisor. The content herein is based on current research and understanding of fibromyalgia as of the publication date, and may not reflect the most recent medical advances or legal changes.
Readers are encouraged to seek professional guidance tailored to their specific circumstances. Neither the author nor the publisher assumes any liability for any loss or damage resulting from reliance on the information contained in this blog post. Always consult with a healthcare professional for medical advice and a legal advisor for legal matters.